 Quick Links
Quick Links
Last night my 3-year-old was up vomiting mucous and alternating high fever and sweaty sleepy periods. She has flu—not a surprise: it is at its peak this season and we’ve been inundated at clinic. Every time my children have a febrile illness, and I watch their fast breathing, their precious sweaty heads and sad coughs, I indulge a bit of thought for parents in years past who battled much more devastating illness. I’ve always loved the history of medicine, partly because it informs the kind of medicine I practice and partly because I love to imagine how people lived.
During nights up with small sick children, I think most often about the terror of diphtheria, a bacteria which causes a thick covering of pus and mucous membrane to the throat and killed children in the millions. This death was horrific—parents watched their children die while fully conscious of suffocation secondary to sloughing debris in their small airways. The cough was violent and families might lose all their children in the course of a few days. And sit by the bed, helpless, much like I was last night, but while their child battled a truly scary foe (unlike the flu, which can be scary, but in an immunized child is very rarely a deathly illness).
During my residency, the Chief Administrative Officer of the Floating Hospital for Children (part of Tufts Medical Center), Dr. John Schrieber, who was also a pediatric infectious diseases physician, would tell residents we were practicing pediatrics, a “wildly successful enterprise of the 20th century.” We were “winning” and had picked a career which was “winning it.” By all measures, he is accurate. Despite recent immunization naysayers who have compromised our success, pediatrics is doing fabulously in the developed world. Deaths of children dramatically declined during the 20th century. If our goal is to save lives, as a profession, we are saving millions and millions of lives, which would have been afterthoughts a century ago. While sanitation and greater access to nutritious foods has played a role in decreasing infectious disease, immunization and development of antibiotics have absolutely revolutionized our care of children.
Let’s take diphtheria as an example. In the small Puritan cemetery across from my Boston apartment during residency, the majority of sad 17th and early 18th century headstones belonged to children, many without names, having died before the age of 1. Many had descriptions of death- and in 1730, a diphtheria outbreak in New England killed a THIRD of children under 10. Those gravestones will sometimes list “suffocation” or “loss of breath.” Parents didn’t just chalk it up to whatever kills most of their children. The quantified it. They enumerated symptoms. And they inscribed it for future generations to see. Later, Victorians termed diphtheria “the strangler.”
An antitoxin was developed from horse serum in the late 19th century and, while it could induce occasionally serious side effects, it could decrease some of the symptoms and lessen disease. It was difficult to produce and expensive and was of limited, if significant, clinical benefit. Notably, charlatans marketed fake antitoxin in large numbers to desperate parents. And with limited expensive supplies, doctors and parents record stories of the heartbreak of picking which children would receive the antitoxin and which children not.
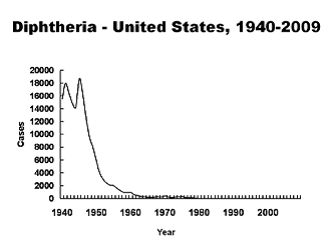
After development of a toxoid vaccine in 1920s and wide availability in the 1930s, diphtheria was virtually wiped out in the U.S. and Canada by midcentury. In the 1990s, as the Soviet Union opened its poorly immunized population to outsiders, it experienced widespread outbreaks of diphtheria. Since then, it is still common in certain parts of the world and without inclusion in our current TDaP and DTaP vaccines, would easily re-emerge in the developed world.
My heart breaks for parents of times past, and I feel so lucky to practice pediatrics and parent in our current optimistic environment for the health of children. Certainly infectious diseases can raise their ugly heads and kill children, even immunized children. They do all the time, even with ventilators and systemic antibiotics and the beginning of some useful antivirals. But the rarity of death from epidemic in the pediatric population in the United States is a huge cause for celebration. My profession is winning. And the challenge of bringing these benefits to undeveloped countries and preventing monsters like diphtheria from the past from returning dominates current discussion.
In the meantime, hug your babies, be thankful to be alive during this amazing time for the health of children and be sure to call us if their bout with flu is more severe or lasts longer than predicted.

My daughter, Ruthie, batting flu with the help of the Paw Patrol and her very own box of Kleenex.

Last night my 3-year-old was up vomiting mucous and alternating high fever and sweaty sleepy periods. She has flu—not a surprise: it is at its peak this season and we’ve been inundated at clinic. Every time my children have a febrile illness, and I watch their fast breathing, their precious sweaty heads and sad coughs, I indulge a bit of thought for parents in years past who battled much more devastating illness. I’ve always loved the history of medicine, partly because it informs the kind of medicine I practice and partly because I love to imagine how people lived.
During nights up with small sick children, I think most often about the terror of diphtheria, a bacteria which causes a thick covering of pus and mucous membrane to the throat and killed children in the millions. This death was horrific—parents watched their children die while fully conscious of suffocation secondary to sloughing debris in their small airways. The cough was violent and families might lose all their children in the course of a few days. And sit by the bed, helpless, much like I was last night, but while their child battled a truly scary foe (unlike the flu, which can be scary, but in an immunized child is very rarely a deathly illness).
During my residency, the Chief Administrative Officer of the Floating Hospital for Children (part of Tufts Medical Center), Dr. John Schrieber, who was also a pediatric infectious diseases physician, would tell residents we were practicing pediatrics, a “wildly successful enterprise of the 20th century.” We were “winning” and had picked a career which was “winning it.” By all measures, he is accurate. Despite recent immunization naysayers who have compromised our success, pediatrics is doing fabulously in the developed world. Deaths of children dramatically declined during the 20th century. If our goal is to save lives, as a profession, we are saving millions and millions of lives, which would have been afterthoughts a century ago. While sanitation and greater access to nutritious foods has played a role in decreasing infectious disease, immunization and development of antibiotics have absolutely revolutionized our care of children.
Let’s take diphtheria as an example. In the small Puritan cemetery across from my Boston apartment during residency, the majority of sad 17th and early 18th century headstones belonged to children, many without names, having died before the age of 1. Many had descriptions of death- and in 1730, a diphtheria outbreak in New England killed a THIRD of children under 10. Those gravestones will sometimes list “suffocation” or “loss of breath.” Parents didn’t just chalk it up to whatever kills most of their children. The quantified it. They enumerated symptoms. And they inscribed it for future generations to see. Later, Victorians termed diphtheria “the strangler.”
An antitoxin was developed from horse serum in the late 19th century and, while it could induce occasionally serious side effects, it could decrease some of the symptoms and lessen disease. It was difficult to produce and expensive and was of limited, if significant, clinical benefit. Notably, charlatans marketed fake antitoxin in large numbers to desperate parents. And with limited expensive supplies, doctors and parents record stories of the heartbreak of picking which children would receive the antitoxin and which children not.

After development of a toxoid vaccine in 1920s and wide availability in the 1930s, diphtheria was virtually wiped out in the U.S. and Canada by midcentury. In the 1990s, as the Soviet Union opened its poorly immunized population to outsiders, it experienced widespread outbreaks of diphtheria. Since then, it is still common in certain parts of the world and without inclusion in our current TDaP and DTaP vaccines, would easily re-emerge in the developed world.
My heart breaks for parents of times past, and I feel so lucky to practice pediatrics and parent in our current optimistic environment for the health of children. Certainly infectious diseases can raise their ugly heads and kill children, even immunized children. They do all the time, even with ventilators and systemic antibiotics and the beginning of some useful antivirals. But the rarity of death from epidemic in the pediatric population in the United States is a huge cause for celebration. My profession is winning. And the challenge of bringing these benefits to undeveloped countries and preventing monsters like diphtheria from the past from returning dominates current discussion.
In the meantime, hug your babies, be thankful to be alive during this amazing time for the health of children and be sure to call us if their bout with flu is more severe or lasts longer than predicted.








